In this post, Julie Zook and I sit down to discuss some key headlines of our recent co-edited book, The Covert Life of Hospital Architecture, which was published open access with UCL Press on 22 March 22.
Health as social, hospitals as social
We conceived The Covert Life of Hospital Architecture in late 2019, just months before the world closed down for the first pandemic wave. The book has just been published as we go into year three of the pandemic. On this bleak anniversary, we in the design professions are being forced to reckon with something that has been foundational for our colleagues in public health all along: individual health is conditioned by social context. Health is social. Our book picks up a small corner of what the social logic of health means for designers by specifically examining hospital spaces. It asks, “How can design best support the functional and social life of hospitals?” Like health, work is social, and the work of hospitals is to restore or manage health.
While we are glad to contribute to the so-called evidence for design decisions, our approach was a little bit different than is typical for evidence-based design. Evidence-based design tends to look at discrete variables and their effects on a per-individual basis. Even when a lot of people are included in a study, they are often (though certainly not always) studied for their impressions or responses with the individual as the unit of analysis. We were more often than not interested in a social unit of analysis. If hospital architecture exists to channel flows of people, things and information, aren’t hospitals there to structure relationships? Individual-level analysis is not always a good tool for understanding these flows.
If hospital architecture exists to channel flows of people, things and information, aren’t hospitals there to structure relationships?
The opening chapter, authored by Julie, covers these arguments, and introduces space syntax as a program for floorplan analysis that recurs in each of the three research chapters. We made two decisions in organizing the book. First, we decided to cope with the different users and multiple overlapping scales of hospitals by spotlighting specific dyads: the patient and visibility that emanates from the patient room, the nursing unit and layout properties that support care team visibility, the visitor and the intelligibility of the public corridor system. We themed these chapters as “pillow”, “table”, and “hallway”. We also invited George Tingwald, Upali Nanda, and Carlo Giannasca—all design professionals—to comment by essay on each chapter.
Nurse surveillance as a team sport that depends on design

Michelle Ossmann was an ICU nurse practitioner prior to getting a Ph.D. in architecture with a focus on environmental psychology. She knew from experience that nurse lore pegged certain out-of-sight rooms as “death rooms”, and that nurses avoided putting the most vulnerable patients in them. She introduced this idea to her doctoral cohort, who studied patterns of movement on the ICUs she had worked in. Michelle developed the concepts of teams, surveillance, and visibility further. She pulled carefully matched chart data on ICU mortality that showed a correlation between a precise patient visibility measure she created and lowered death rates.
Amplifying design for team-based knowledge work among nurses
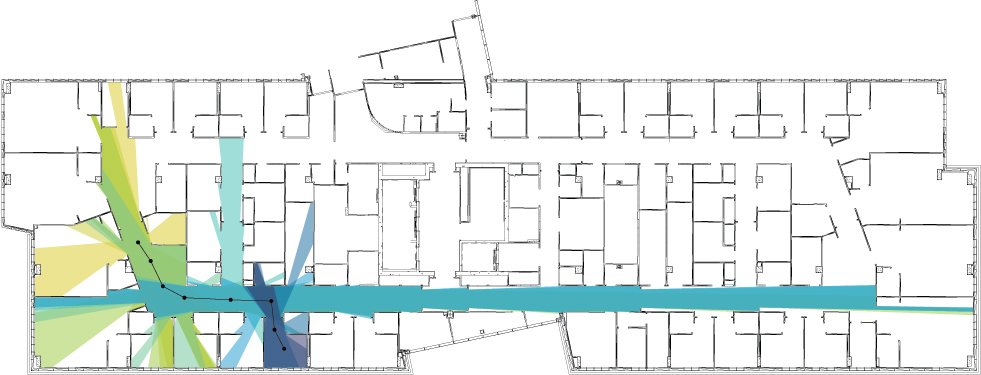
Rosica Pachilova completed her Ph.D. in architecture under my supervision. My own research background was primarily in design and workplace behavior, especially for knowledge work settings. Even as nurse work becomes more complex and collaborative, the status of nurses as knowledge workers is often underemphasized when we design hospitals. One can see this in the decades of studies focused on design for task efficiency, which is not a bad thing, but is also not the whole picture. Rosica and I turned this approach upside down. Rather than asking, “how short is the nurse path”, our research asked, “how enriched with opportunities to collaborate is the nurse path?” We developed a novel measure to assess this, and preliminary data indicates that more collaboration-friendly units might better support quality of care.
Preventing the ugly and confusing corridor system by design
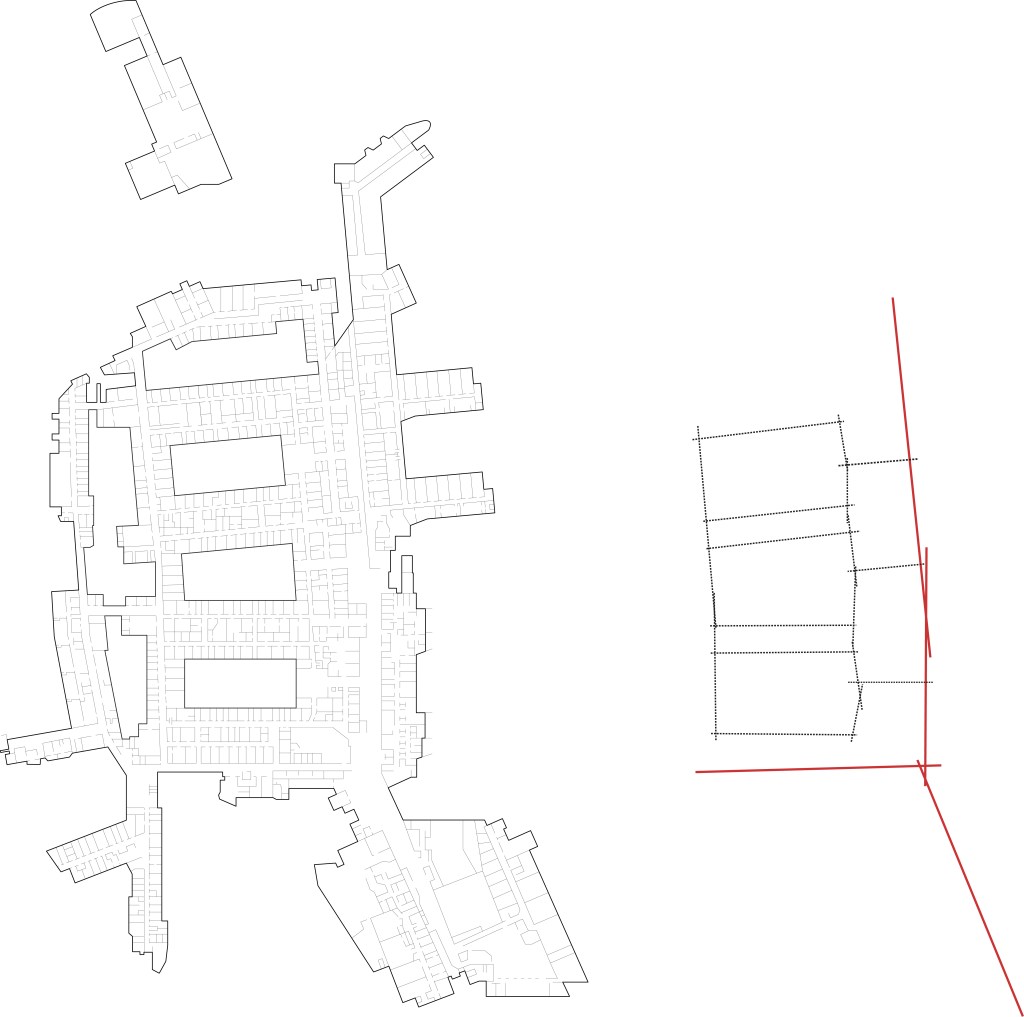
Sonit Bafna and Julie revived the old problem of the confusing hospital corridor system, especially as faced by a visitor. They asked, “What design properties make a corridor system intelligible?” They carefully unpacked the point that the so-called cognitive map is a metaphor, and not a literal map in the head. With this clarification, they were better able to focus on specific floorplan layout guidelines, some of which run counter to received wisdom on wayfinding. Further, contra trends to suppress the identity of hospitals as institutions, they assess how corridors can constructively convey institutional character to the visitors and patients who come to them seeking care.
Dilemmas in togetherness and isolation
In the closing reflective chapter, I take on the challenge of evaluating the pandemic response in the UK and China to draw conclusions about wider trends in healthcare design. The social aspects come to the fore here as the pandemic has upended many hard and fast beliefs of how to avoid spread of a deadly disease, of how to give care, of how to work together, of how to be human, of how to be together with others in difficult times. These insights are then brought back to the themes raised in the previous chapters, i.e., which user (collective) to consider and how to link to bridge research and practice.
We hope the book shows how subtle aspects of space as experienced hold out promising links to outcomes in hospitals. We wrote (and illustrated) the book to make this specialist literature accessible to a range of professionals and academics as well as to general readers, and we hope this knowledge finds its way into their hands.
The Covert Life of Hospital Architecture can be downloaded as a free pdf from University College London Press here: https://www.uclpress.co.uk/products/178413







Pingback: The Covert Life of Hospital Architecture — spaceandorganisation — FREE BOOK | lifeunderwriter.net